The Ileocecal Valve: A Hidden Key to Gut and Back Health
The ileocecal valve (ICV) is an essential yet often overlooked component of digestive health. Situated between the small and large intestines, this valve plays a crucial role in regulating the passage of intestinal contents and preventing backward flow. When functioning properly, it opens briefly to allow digested material to move into the colon before closing again to prevent reflux. However, dysfunction of the ICV can lead to a host of digestive and systemic issues, including lower back pain, small intestinal bacterial overgrowth (SIBO), and upper gastrointestinal symptoms.
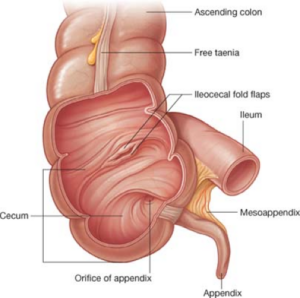
How the Ileocecal Valve Affects Lower Back Pain
One surprising consequence of ICV dysfunction is its potential impact on lower back pain. The ileocecal valve is located in the lower right quadrant of the abdomen, near the appendix. When the valve becomes irritated or inflamed, it can cause referred pain to the lower back and pelvis. This is often mistaken for musculoskeletal issues, leading to ineffective treatments that do not address the root cause.
The connection between the gut and musculoskeletal system is facilitated by the nervous system, particularly through the vagus nerve and spinal segments that share innervation with the intestines. Chronic ICV dysfunction can lead to persistent lower back discomfort, making it crucial to consider digestive health in cases of unexplained back pain.
ICV Dysfunction and SIBO
SIBO, a condition characterized by excessive bacteria in the small intestine, is closely linked to ICV dysfunction. When the valve fails to close properly (remaining open), bacteria from the colon can migrate back into the small intestine, disrupting its normally low bacterial environment. This can result in symptoms such as bloating, gas, diarrhea, and malabsorption of nutrients. Conversely, a stuck-closed ICV can contribute to stagnation, slowing the movement of intestinal contents and potentially leading to constipation and fermentation of undigested food, which can further exacerbate bacterial imbalances.
The ICV and Upper GI Symptoms
Though the ileocecal valve is located in the lower digestive tract, its dysfunction can manifest in upper GI symptoms such as bloating, acid reflux, nausea, and burping. This occurs due to the disrupted flow of digestion, which can cause food to remain in the stomach and small intestine longer than intended. Additionally, inadequate closure of the valve may contribute to excessive fermentation, leading to increased gas production and discomfort.
Causes of ICV Dysfunction
Several factors can contribute to ICV dysfunction, including:
- Dietary Factors: A diet high in processed foods, inflammatory grains, refined sugars, alcohol, caffeine, and artificial additives can irritate the gut lining and affect valve function. On the other hand, insufficient fiber and whole food nutrition can impair proper motility.
- Digestive Imbalances: Low stomach acid, enzyme deficiencies, and conditions such as exocrine pancreatic insufficiency (EPI) can hinder digestion, leading to undue stress on the ICV.
- Stress and Emotional Trauma: The gut-brain axis plays a significant role in digestive function. Emotional distress, chronic stress, and unresolved trauma can dysregulate the nervous system, affecting ICV motility.
- Antibiotic Overuse and Dysbiosis: Prolonged use of antibiotics and other medications can disrupt the gut microbiome, leading to dysbiosis that contributes to chronic ICV dysfunction.
- Surgical History: Appendectomies and other abdominal surgeries may alter the function of the ICV, particularly if scar tissue forms in the surrounding area.
Recognizing ICV Dysfunction
While symptoms can vary widely, common signs of ICV dysfunction include:
- Chronic bloating and abdominal discomfort
- Unexplained lower back pain
- Alternating diarrhea and constipation
- Fatigue and brain fog
- Acid reflux or heartburn
- Food sensitivities and poor digestion
Addressing ICV Dysfunction
Restoring proper function to the ileocecal valve requires a multi-faceted approach:
- Dietary Modifications: Focus on a balanced diet rich in fiber, whole foods, and adequate protein while avoiding processed and inflammatory foods.
- Digestive Support: Supplementing with digestive enzymes, betaine HCl, or probiotics may help restore balance.
- Stress Management: Practices such as meditation, breathing exercises, and vagus nerve stimulation can improve gut-brain communication.
- Fascial Counter-strain: Addressing the dysfunction/inflammation with fascial counterstrain. Targeting the underlying fascial restrictions, lymphatic congestion, and neural dysfunction associated with this area. The ileocecal valve, which regulates the passage of contents from the small intestine to the large intestine, can become dysfunctional due to inflammation, visceral restrictions, or autonomic nervous system dysregulation. FCS specifically targets protective reflexes within the fascia, helping to reduce tension and improve the mobility of the valve and surrounding structures. By releasing strain patterns in the lymphatic, vascular, visceral, and nervous system components connected to the ileocecal valve, FCS may help restore normal motility and function. This can lead to improvements in symptoms like bloating, constipation, diarrhea, right lower quadrant pain, and systemic issues related to gut dysbiosis or immune dysfunction.
Final Thoughts
ICV dysfunction is an often-overlooked contributor to digestive distress, chronic pain, and systemic imbalances. By recognizing the signs and addressing the root causes, individuals can take proactive steps to support their gut health and overall well-being. If you suspect ICV dysfunction, book an appointment today.
